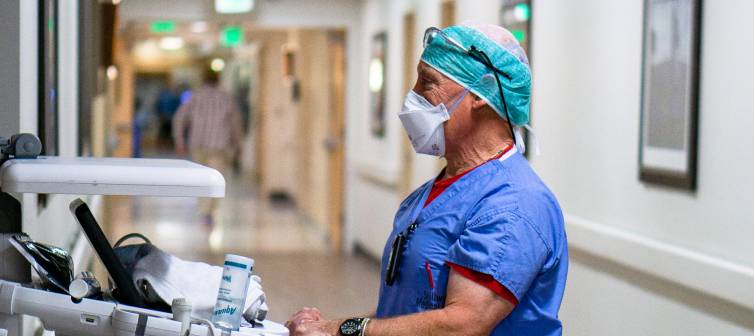
Find the Service You Need
Although medical services are the way we care for people, we also believe that a community hospital provides a unique opportunity to care about people. For every stage of your life and every need your family has, we welcome you as our neighbors, fellow community members and friends – and treat you with innovative medicine right here at home. We welcome you to discover why we say that the size of the hospital has nothing to do with the size of the care.